“The host site, the artery in this case, is an excellent source of cells and provides a very efficient growth environment. This is what inspired us to skip the cell culture altogether and create these cell-free synthetic grafts.”
In short
Researchers at University of Pittsburgh have developed a cell-free, biodegradable artery graft which they claim is absorbed by the body after having acted as a scaffold for a new artery. If that can be established in humans the group believe it could potentially transform coronary artery bypass surgery because within 90 days of surgery the patient will have a regenerated artery with no trace of synthetic graft materials left in the body.
Background
Research published online June 24 in Nature Medicine highlights work led by principal investigator Yadong Wang, a professor in Pitt’s Swanson School of Engineering and the School of Medicine’s Department of Surgery, who designed grafts that fully harness the body’s regenerative capacity. The result is a graft made from an elastic, absorbable polymer called Poly(glycerol-sebacate) (PGS), that is surrounded by a fibrous sheath to trap cells and then coated with heparin to bind growth factors and prevent clotting.
They claim this new approach is a philosophical shift from the predominant cell-centered approaches in tissue engineering of blood vessels.
Researcher comments
“The host site, the artery in this case, is an excellent source of cells and provides a very efficient growth environment,” said Wang. “This is what inspired us to skip the cell culture altogether and create these cell-free synthetic grafts.”
“The results were porous grafts that are suturable,” said Wang. “And the rapid remodeling of the grafts led to strong and compliant new arteries. The extent of the changes in the grafts that occurred in just 90 days was remarkable.”
In vivo confrmation
Wang and his colleagues made grafts as small as 1 mm in diameter and monitored the graft’s transformation in vivo for three months. Because the graft was highly porous, cells were easily able to penetrate the graft wall, and mononuclear cells occupied many of the pores within three days. Within 14 days, smooth muscle cells—an important blood vessel builder—appeared. At 28 days, cells were distributed more evenly throughout the graft. At 90 days, most inflammatory cells were gone, which correlated with the disappearance of the graft materials. The artery was regenerated in situ and pulsed in sync with the host. Furthermore, the composition and properties of the new arteries are nearly the same as native arteries.
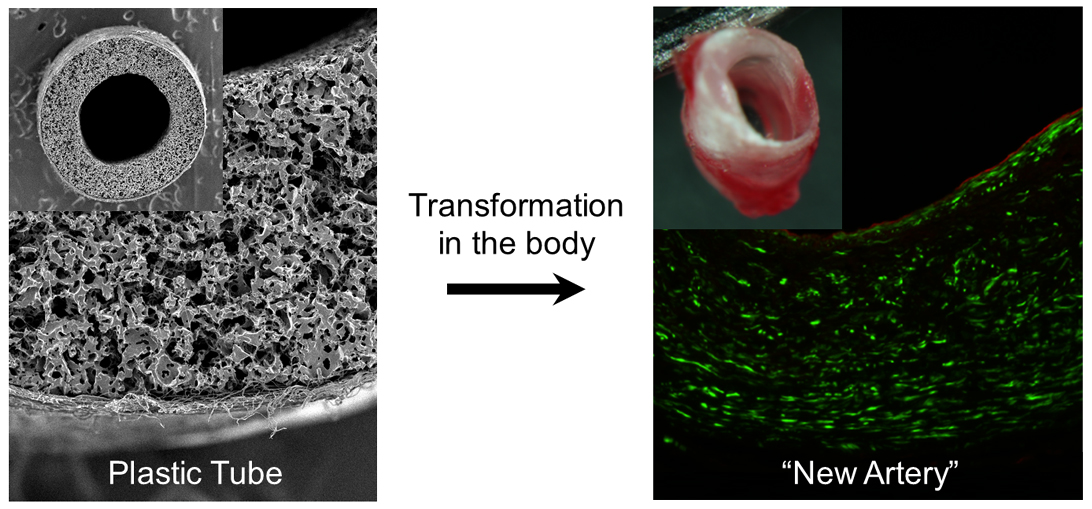
“This report is the first that shows a nearly complete transformation of a synthetic plastic tube to a new host artery with excellent integration within three months,” said Wang. “Most likely, the amount of time it takes to regenerate an artery can be further shortened as we refine the system.”
Current approaches toward tissue-engineered arteries require a long production cycle because of the required cell culture steps. The newly developed graft is made in a few days, stores in a dry pouch at ambient temperature, and is readily available off the shelf. The ease of use and storage are similar to the conventional Dacron® grafts.
Source: University of Pittsburgh
published: June 28, 2012 in: Cardio, Technology, Universities, Vascular
